What’s the deal with fiber? What are the benefits of eating more of it? Does it matter which kind of fiber you eat?
One notable feature of dietary fiber is that your body (mostly) doesn’t digest it. What relationship that has to its supposed health benefits, I can only guess. As a type-1 diabetic with an insulin pump and a continuous glucose monitor, I know that my morning Fiber One bar has 29 grams of carbs, but 9 are fiber and I only take insulin for the other 20 carbs. If I take insulin for all 29, my blood sugar goes too low.
Google Scholar brings up some strong evidence for dietary fiber. Nutritional studies are typically low quality, but there have been a very large number of randomized controlled trials (RCTs) of increasing your dietary fiber intake. They’re all short-term, but most nutritional studies rely entirely on observational evidence, so it’s an impressive state of affairs.
Blood Pressure
This meta-analysis of 25 randomized controlled trials (RCTs) measured the benefit of eating more dietary fiber for blood pressure. Overall, they found small reductions in blood pressure as a result of eating more dietary fiber. Five of the trials were specifically in people who had high blood pressure to begin with. For those people, the high fiber treatment reduced their systolic blood pressure (the top number) by about 6 mmHg. Interventions that lasted longer than eight weeks or had larger doses of fiber – more than an 8 gram per day increase versus baseline – had larger benefits. This meta-analysis also found larger benefits for people over 40. Reducing your blood pressure by 6 isn’t huge, but it’s meaningful for such a minor change in behavior.
Blood Cholesterol
This meta-analysis specifically looked at 67 RCTs of soluble fiber and found a modest but statistically significant benefit for lowering LDL cholesterol. Eating about 3 servings of oatmeal a day would reduce your LDL cholesterol by about 2.3 mg/dL. Such a large number of RCTs makes for very high quality evidence, but that benefit is small.
Weight Loss
This review article (I can only read the abstract, full text behind a paywall) says that RCTs have found that adding 14 g/day of dietary fiber causes people to lose about 4 pounds over 4 months. In lab tests, when people are allowed to eat as much as they want, they eat less when the food is high in fiber. If they’re given meals of equal calorie count, they report being less hungry after eating a high fiber meal. People who have more weight to lose lose more weight on high-fiber diets. It doesn’t seem to matter whether the fiber comes from foods that naturally have lots of fiber or from a supplement.
Cardiovascular Disease
The above results are all from randomized trials, which means we can be confident it’s causal, but the tradeoff is these trials all have to be relatively short term. That’s why they only measure intermediate outcomes like blood pressure and not the bigger outcomes like heart attacks or death. For these bigger, rarer outcomes, we have to turn to observational studies.
The Women’s Health Study was an experiment that surveyed 40,000 female health professionals on their eating habits and randomly assigned them to take aspirin or a placebo. Along with the related Nurses’ Health Study and Physicians’ Health Study, these surveys of tens of thousands of people give us some of the highest quality observational datasets on diet and health outcomes.
This prospective study used data from the Women’s Health Study to see if women who had higher fiber diets had a lower risk of cardiovascular disease. They did. The people who ate more fiber also exercised more and smoked less, so we can’t attribute all the difference to the fiber. After adjusting for a bunch of other factors, the study found a 20% reduction in cardiovascular disease and a 30% reduction in heart attacks, but with such wide error bars it isn’t statistically significant.
To facilitate comparison, this study and others like it calculate the reduction in CVD risk for a 10 gram increase in dietary fiber per day. Meta-analysis of this calculation across 10 large studies finally gives an overall 17% reduction in CVD risk
| Study | CVD Risk Reduction per +10 g/day of Dietary Fiber |
| Women’s Health Study (40,000 women) | 17% |
| Health Professionals Follow-up Study (44,000 men) | 19% |
| Nurses’ Health Study (69,000 women) | 19% |
| Alpha-Tocopherol, Beta-Carotene Cancer Prevention Study (22,000 male smokers) | Okay, they didn’t do this calculation, but they still found fiber is good for CVD |
| Meta-analysis of 10 studies | 17% (95% confidence interval: 11% – 22% reduction) |
Take note, Paleo diet fans: the three studies listed after the WHS found that cereal fiber, like that found in bread and pasta, had a larger effect than fiber from fruits and vegetables. Really it’s hard to say much about which kind of fiber is best because they’re all correlated with each other, but this makes me more skeptical than I already was of the Paleo/gluten-free craze.
The WHS paper notes that the large benefits found in observational studies are incongruous with the tiny benefits for cholesterol and blood pressure found in experiments. It could be that following a high-fiber diet for a long time makes a bigger difference than a couple months, or that there are protective mechanisms that the experiments haven’t measured. Measuring the effect of fiber wasn’t the main point of any of these gigantic studies, though, so it’s possible that there’s some publication bias here. If some researchers conducted a secondary analysis of a large experiment and found a null result for the benefit of fiber, they might just choose not to publish. It’s also possible that the way they control for healthy habits aside from eating fiber isn’t sufficient. For example, dietary fiber consumption is correlated with whole grain consumption, and other studies have found that whole grains protect against CVD independent of dietary fiber consumption; the studies analyzed in this paper did not adjust for whole grain consumption.
All Cause Mortality
Now, for the greatest health outcome of all: death. This paper used data from the NIH-AARP Diet and Health Study, which surveyed over 550,000 people between 50 and 71 and followed them for just under 10 years. The researchers found that an incremental 10 g/day of dietary fiber reduced total mortality 12% in men and 15% in women. When they performed the analysis only on never-smokers instead of using a linear adjustment for level of smoking, the benefit got even larger.
Besides an overall reduction in mortality, they found separate, significant reductions in mortality due to cardiovascular disease, cancer, infectious diseases, and respiratory diseases. As an interesting little control, they find no reduction in death due to accidents. If they did, all the results might seem implausible. Since they don’t, the results can’t just be because people who eat more fiber are generally more cautious.
Here are their main results:
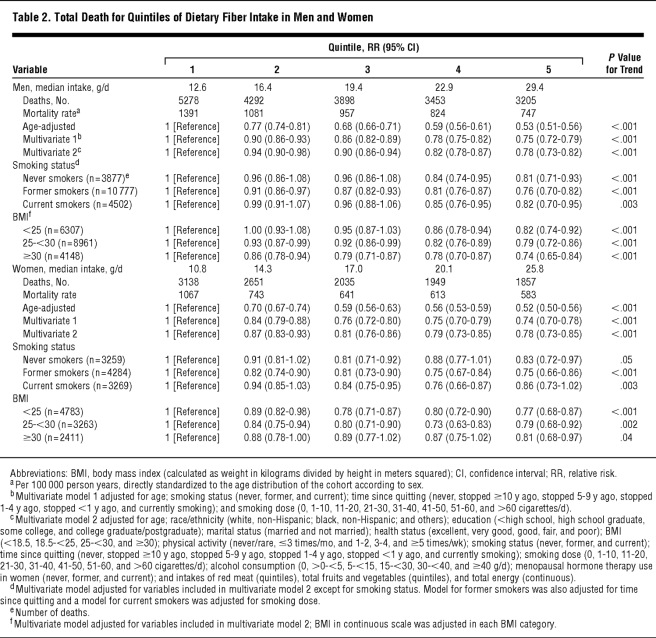
In sum, it seems like there’s a good chance a high fiber diet is good for you. The higher fiber groups in all these studies got about 25 – 30 g / day, in line with the government’s recommendations. That’s what I’d shoot for.

