Like me, you might be a little confused about whether fish oil supplements reduce the risk of heart attacks and strokes. Can fish oil really extend our lives, and is it worth the expense?
Decades of nutritional studies that survey what people eat and measure their health outcomes have found that eating fatty fish is correlated with a decreased risk of dying from heart disease or stroke. Those studies can’t establish cause-and-effect, but they have led to large-scale randomized controlled trials (RCTs) of fish oil supplements that can.
The early RCTs found that fish oil supplements do in fact decrease the risk of cardiovascular disease (CVD). Confusingly, later RCTs didn’t bear that out.
What explains these conflicting results? One idea is that as the public became more aware of the health benefits of fish, people started eating more fish and no longer needed to take supplements. Another idea is that statins confer the same benefits as fish oil, so now that statin use has become common, there’s no further benefit to fish oil.
In this post I’ll look into what the sum total of the evidence says about the cardiovascular benefits of fish oil supplements for people who are generally healthy. I’ll also explore whether statin use or dietary fish intake makes any difference to those benefits.
Lit review of fish oil supplements
All the recent RCTs seem to have been captured in this 2018 meta-study, which includes 13 large, high-quality RCTs of fish oil supplements. Neither I nor this review from January 2020 found any more recent RCTs, so I’ll treat that list of 13 as comprehensive.
One of those RCTs is an oddball, so let’s get it out of the way first. Named REDUCE-IT, it was run as an FDA drug trial, so it followed the strictest guidelines for study design. It monitored 8,000 patients for five years. Two things make it odd. First, it studied people who were taking statins and had low LDL (bad cholesterol) but high triglycerides. Second, the fish oil dose was truly massive: 4 grams daily, which is four times the next highest dose across the 13 RCTs. In addition, it was a highly purified form of fish oil that’s different from what you can get over the counter. The drug successfully reduced triglycerides and caused a huge 25% decrease in heart attacks, strokes, and deaths from CVD. The drug is now approved as Vascepa, available as a prescription to complement statins. But because of its oddness, this study adds only indirect evidence that over-the-counter fish oil supplements are good for the general population.
Now to the other 12 studies. Six of these were great. The other six didn’t measure up quite as well on things like sample size and study design, but they were still good. The data from all 12 are combined in the meta-study I’m relying on, and they show that fish oil supplements significantly decrease heart attacks, heart disease, and their related deaths. With only data from the six great studies , the results get slightly weaker but still point in the same direction. It’s also worth noting that there are conflicting results between individual studies, even if we only look at the six highest-quality ones.
Could the variations in the six great studies be explained by differences in statin use and fish consumption? The meta-study doesn’t check for that, so I’ve done it myself. (One of the six studies is stuck behind a paywall, so I can only include data from the other five.)
Interaction between statins and fish oil supplements
It is plausible that the benefits of fish oil supplements have gone down over time because more people are also taking statins. If that was true, we’d expect to find evidence that people on statins receive less benefit from fish oil than people not on statins.
The table below looks for this evidence. It shows the relative risk of each study’s primary outcome for the fish oil group compared to the placebo group, separated by statin status. A number below one means people taking supplements had a lower risk of the main bad outcome the study was tracking. In other words, below one is good, and I’m asking if statins affect that number. Each study tracked a slightly different primary outcome, but I’ll gloss over those differences and summarize them all as “cardiovascular disease.”
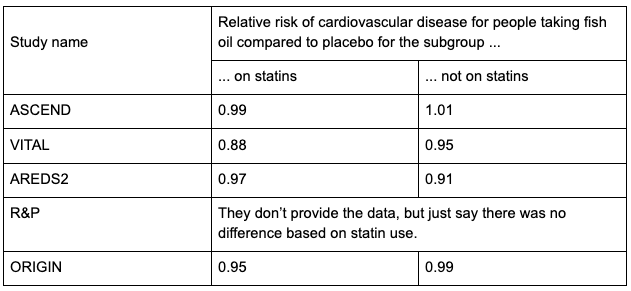
As the table shows, the differences are tiny, and three of the four studies show that people on statins benefited from fish oil more than people not on statins. (None of the differences were statistically significant.) It doesn’t take any fancy math to tell you that these studies do not support the claim that there is an interaction between fish oil and statins.
Interaction between eating fish and taking fish oil supplements
It’s also been suggested that people who eat plenty of fish benefit less from taking fish oil supplements. Four of the studies broke out results separately based on how much fish people ate. The table below looks at those four studies individually and then combines their results using fixed effect meta-analysis.
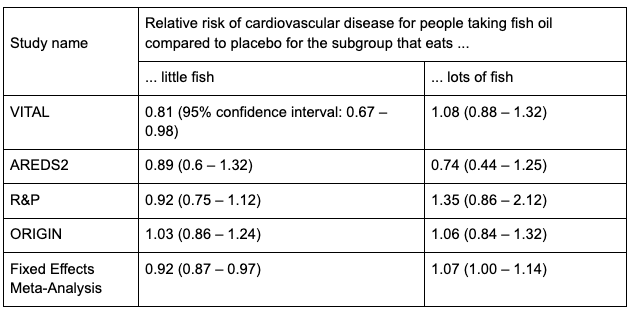
Only the VITAL study found a meaningful difference between the low- and high-fish groups. The other three studies showed no significant difference, so you might guess there’s really no interaction between fish-eating and the effectiveness of fish oil supplementation. But the fixed effect meta-analysis combining the four studies shows us there is a benefit for people with a low-fish diet but not for people with a high-fish diet.
Cost effectiveness for extending life
Supplements can be expensive, so I like to consider how much a little more life expectancy is going to cost. In my post on multivitamins, I estimated that a lifetime spend of about $800 on multivitamins should add about six months to your life expectancy. That’s a bargain. Now I’d like to estimate the cost-effectiveness of taking fish oil supplements for people on a low-fish diet. To do that, I need to convert the effects above to changes in life expectancy.
While the cardiovascular outcomes referenced in the table above include nonfatal heart attacks and strokes, I’m going to make the jump to assuming people on a low-fish diet are 8% less likely to die from CVD if they take fish-oil supplements. As I did with multivitamins and red meat, I’m going to take the Social Security Administration’s survival probabilities by age and adjust them for the estimated benefit of fish oil to calculate the change in life expectancy. But first, I have to convert from a reduced risk of CVD mortality to all-cause mortality.
This page from the CDC provides the top 10 causes of death by age. For each age group, I assume that total mortality decreases by 8%, from the fixed-effects meta-analysis above, multiplied by the fraction of all deaths in that age group caused by CVD (The CDC splits CVD into heart disease and cerebrovascular disease). You can follow my calculation on the ‘Fish Oil’ tab of this Google Sheet.
I find that for a person who eats little fish, beginning fish oil supplements at age 25 extends life by 0.24 years. Delaying until age 35 only reduces the benefit to 0.23 years. The difference of about .01 years, or 4-ish days, might sound like it’s not worth it to start taking fish oil at 25. But fish oil supplements at a dose similar to these studies cost about $0.10 per day. That means that taking fish oil supplements from 25-years-old through 34-years-old buys a statistical year of life for about $36,500. And the older you get, the more beneficial fish-oil pills get. Don’t take the exact dollar value literally, but that’s on par with buying HEPA filters or wearing daily sunscreen and more than a factor of 10 cheaper than the value the FDA places on a statistical life year.
In short, if you don’t eat at least about two servings of fatty fish per week, fish oil supplements are a cost-effective way to extend your life. Make sure the supplements you buy have at least about 500 mg total of EPA and DHA (like this one). These are the ingredients studied in all the trials I’ve considered. Be aware that many fish oil supplements (like this top result on Amazon) have very low concentrations of the ingredients that matter.

